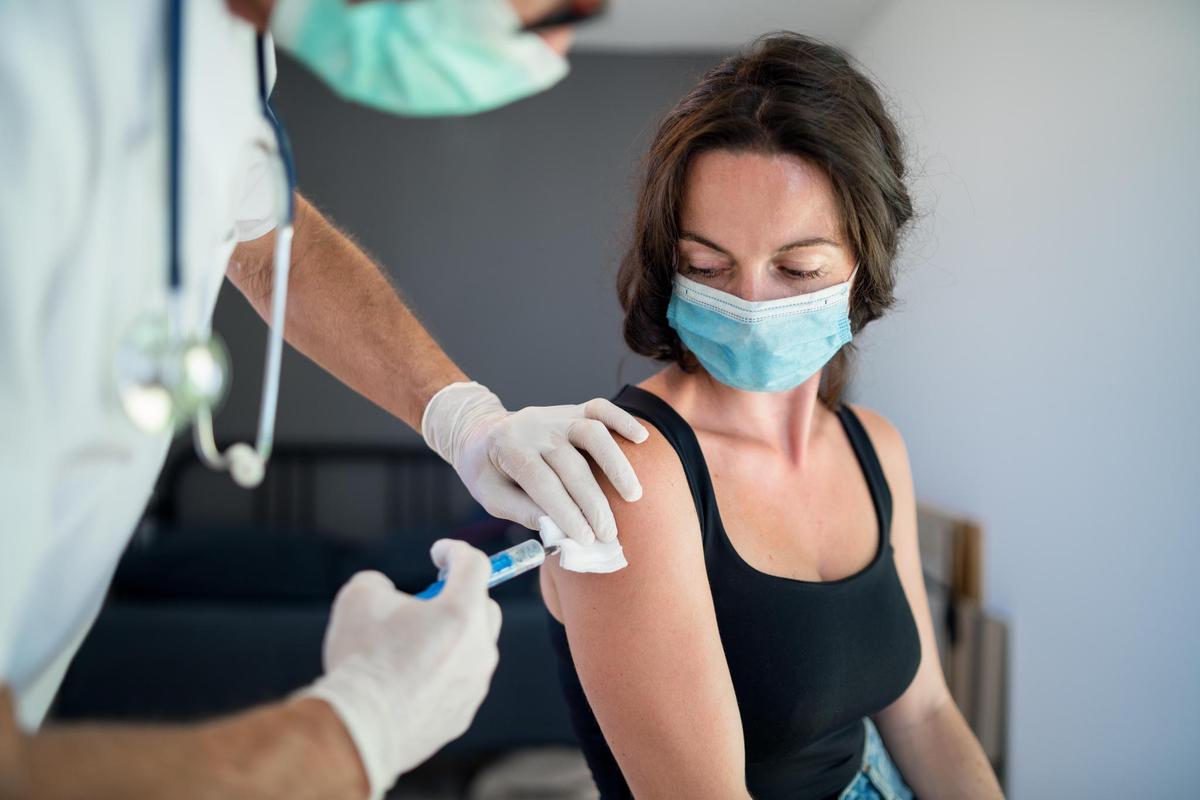
The Delta Variant Is Making COVID-19 a Pandemic of the Young
It has been said countless times by magazines, public health figures and politicians that COVID-19 is now a pandemic of the unvaccinated. The line is easy to write because it’s true. Breakthrough infections among the vaccinated are an issue, the virus lapping at the edges of our collective immunity. But severe illness and death are almost entirely concentrated among those who haven’t yet gotten the shot.
But who are those unvaccinated people? Increasingly, they are the young. The largest group is little kids, those under 12 because no vaccine has been authorized for them. But the picture doesn’t get much better in older children. According to the figures gathered by the Centers for Disease Control and Prevention, only a third of kids aged 12 to 15 in the US are fully vaccinated. The figure remains below average for people in their late teens and twenties.
It’s also a confusing reality. The pandemic rules that were ingrained 18 months ago went roughly like this: The young and less vulnerable are meant to stay home and take other precautions to protect the old and those with preexisting health conditions. This understanding stemmed from the pandemic’s silver lining: that young people are the least likely to develop severe illness that leads to hospitalization or death – an unusual pattern for respiratory disease, which often affects children as well as the old.
Experts like Fisman, an epidemiologist at the University of Toronto, worry that fatigue and lack of emphasis on the risks to kids lead to fewer precautions just as transmission goes up among children. Here are some of the things to know:
Why Hasn’t the Virus Affected Kids as Much as Adults?
Researchers who study the immune system have started to feel more confident with certain explanations in recent months. One difference is that kids appear to have a more battle-ready immune system when a COVID-19 infection begins. That immune response starts with the production of antiviral proteins called interferons, which recruit a battalion of immune cells up to the nose, explains Kerstin Meyer, a principal staff scientist at the Wellcome Sanger Institute who has studied the difference between adult and child responses. One feature of COVID-19 infections in older people is that these initial warning signals are often suppressed, preventing that crucial early response from ramping up. This allows the virus to multiply quickly in the upper airways and then spread deeper into the lungs, where it causes more severe illness. But in children, “this viral sneakiness is prevented,” Meyer says. Cells in the nose and throat appear more primed to mount a quick response, so the infection typically ends before anything more than mild symptoms appear.
Is Delta Making Kids More Sick Than Other Variants?

There’s little evidence so far to suggest the Delta variant is more harmful to children than adults. According to the CDC, there’s some evidence of greater severity in Delta infections across all age groups, but the agency has yet to offer a specific breakdown for children. In Ontario, where Fisman has been tracking the hospitalization rate among young people, children under ten infected with Delta have been more than twice as likely to be hospitalized as those infected with other variants. But the data is still relatively sparse – in the province, there are 1,300 cases in kids under ten and only 26 hospitalized – and there are too few cases to estimate the relative risk of ICU admission or death. But Fisman’s confidence in his conclusion is rising as more data comes in. “The stakes are a little bit higher for keeping this away from kids,” he says.
Where Is This All Heading as the School Year Begins?
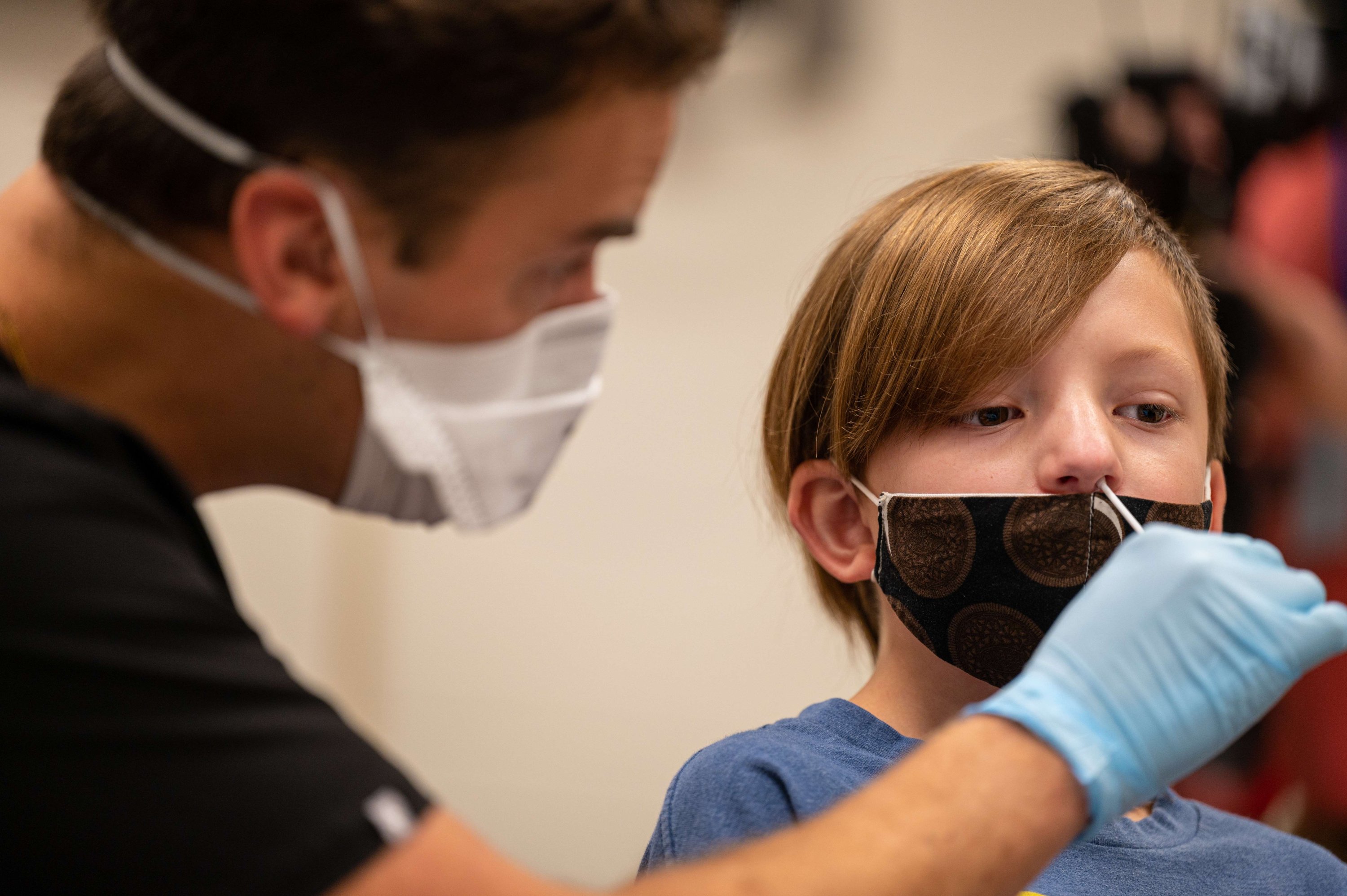
The most powerful tool remains vaccination, says Permar, chair of pediatrics at Weill-Cornell Medicine and New York-Presbyterian Komansky Children’s Hospital. She has called on the Food and Drug Administration to offer a clear and expedited timeline to make shots available for kids younger than 12. But in the interim, the same basic principles that have applied throughout the pandemic also apply to controlling Delta. She notes that her New York hospital has seen a steady trickle of cases of COVID-19 or RSV but so far, not the surge seen in the south. She attributes the difference to prevalent mask-wearing and relatively high rates of vaccination. Vaccinated adults help create a protective cocoon around kids who can’t get the shots.
But even in places where other preventative measures like testing regimens and ventilation overhauls worked for schools that remained open in the spring, these options may no longer do the trick with a more transmissible variant. Fisman also points out that school administrators may have dropped their guard thinking the pandemic was essentially over, perhaps investing less in ventilation or dropping mask requirements in class or testing protocols.
Let us know in the comment section your thoughts about the pandemic is affecting kids.
You May Also Like

Exploring Science and Miracles
2023-12-26
Top 6 NASA Inventions That Changed Our Lives Forever
2023-04-17